As health care reorganization occurs at the federal level, local and regional efforts can serve as models that can accelerate improvement toward achieving better population health and better care at lower cost. In the paragraphs below we describe several initiatives in Michigan that can serve as examples of the direction cardiovascular care delivery will need to move in this new era of the Affordable Care Act. These programs pursue better health outcomes at lower cost by the application of better evidence-based care, the utilization of regional quality improvement collaboratives, community-based childhood wellness promotion, and medical device-based competitive bidding strategies.
Over the past 15–20 years, it has been apparent that cardiovascular care expenditures are proportionally higher than the benefit in cardiovascular risk reduction in the United States. Perhaps one of the most obvious areas is the use of cardiac imaging stress tests and coronary artery angioplasty (Figures 4 and 5). Despite the steadily increasing use of stress testing and percutaneous coronary intervention in stable coronary disease, there has been no impact on hospitalization for acute heart attack.16 The COURAGE trial and other similar investigations have proven that, with excellent medical therapy, the routine use of stress testing and percutaneous coronary intervention for stable coronary disease has no impact on either survival or acute MI.17 In the United States, the “weaning” from this financial stream related to routine stress testing followed by elective coronary intervention is ongoing and should result in substantial savings.18
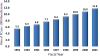 | Figure 4. Temporal Changes in Rates of Cardiac Percutaneous Coronary Intervention (PCI) per 1000. |
 | Figure 5. Trends in Population-based Hospitalization for AMI and Stress Testing among Medicare Beneficiaries 1993-2001, Adjusted for Age, Gender, and Race. |
A Systematic Approach to the Application of Evidence-Based Care to Improve Outcomes and Cost
Recognizing this area for improvement, teams at the University of Michigan have focused on applying the perioperative cardiac care guidelines to patients being considered for elective aortic surgery.
19 As outlined in
Table 3, by implementing a national guideline that carefully outlines the indications for stress testing, coronary angiography, and coronary intervention prior to elective aortic aneurysm repair, caregivers both reduced cost and improved outcomes through the use of evidence-based practice guidelines. A focus on implementing evidence-based care strategies will allow the US health care system to achieve better outcomes for its expenditures.
 | Table 3. Resource Use and Outcomes after Implementation of American College of Cardiology/American Heart Association Preoperative Risk Assessment Guidelines. |
By improving the systems through which evidence-based care is delivered, the Guideline Applied in Practice project in Michigan improved post-MI care over a 10-year period. By involving 400 cardiologists, 33 hospitals, and teams of physician and nurse leaders, the Guideline Applied in Practice project proved that embedded reminders into care processes aimed at the effective use of early aspirin, beta blocker and LDL measurement, ACE inhibitors, smoking counseling, cholesterol treatment, and dietary counseling improved the performance measures during acute coronary syndrome care.20–22 Most importantly, the study demonstrates this practice has a favorable impact on mortality after MI in Medicare beneficiaries, lowering the in-hospital mortality from 13.6% to 10.4%, and the one-year mortality from 38.3% to 33.2% (Figure 6). This effort illustrates that by measuring care on a regular basis, interventions can be identified to improve systems and quality in a sequential and iterative basis through rapid-cycle quality improvement. The ability to identify defects and rapidly improve outcomes will allow health systems to respond with agility in the new health care environment.
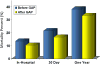 | Figure 6. American College of Cardiology Guidelines in Applied Practice for Acute Myocardial Infarction (ACC GAP AMI) Program Mortality Benefit in Medicare Patients. |
Utilizing Regional Quality Improvement Collaboratives
A similar approach is taken at a larger scale in The Blue Cross Blue Shield of Michigan Cardiovascular Collaborative (BMC2) quality improvement collaborative.
23,24 In this program, all process and outcome measures of the state’s coronary interventions are documented and entered in a central core laboratory that produces regular reports for operators and hospitals. Through their efforts, the BMC2 investigators identified a maximum allowable contrast dose for patients undergoing an angioplasty that predicted a 6-fold risk increase in the development of acute renal failure.
25 By implementing a strategy where the maximum allowable contrast dose was calculated before a patient underwent angioplasty in each hospital, the investigators were able to achieve a significant reduction in the frequency of dialysis-dependent renal failure after coronary intervention (
Figure 7).
26 This is an example of the detection and prevention of a relatively infrequent but severe complication related to care processes that would have gone undetected without a large collaborative study. This model in Michigan can be readily duplicated by other states, and the Affordable Care Act is likely to lead to similar large regional and national consortia for improving care and preventing harm.
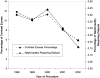 | Figure 7. Percentage of Patients Exceeding the Maximum Weight and Creatinine-adjusted Contrast Dose, and Percentage of Patients Developing Nephropathy Requiring Dialysis. |
Investing in Community-Based Health and Wellness Promotion
By emphasizing prevention and investing in its community, the University of Michigan has been successful in improving the health status of children across the state. The Project Healthy Schools initiative in Michigan targets middle schools with an intervention to improve childhood health. Eagle and colleagues have demonstrated through a number of studies that by developing an educational curriculum in middle schools, improving cafeteria offerings, and changing beverages and snacks sold in vending machines to healthier choices, the health status of middle school children can improve.
27 In the Michigan experience, this improvement is seen within 10 weeks of the intervention and is sustained over a period of three years.
28 The fast food and electronic gaming revolution has created a generation of young people who are overweight, unfit, and much more likely to develop hypertension, diabetes, and coronary disease later in life. Project Healthy Schools is one example where investing in community health has the opportunity to prevent long-term adverse cardiac events. This partnership with communities can be easily modeled by other health systems in this era of health reform.
Reducing Health Care Costs through Competitive Bidding Strategies for Medical Devices
Emanuel and colleagues have written that transparency in the cost of care and a focus on improving supply line costs have the potential to reduce the cost of care delivery through competitive bidding strategies.
29 In cardiovascular care delivery, pacemakers, defibrillators, coronary catheters, stents, and cardiac valves are a remarkable source of cost. At the University of Michigan, the interventional teams in cardiac surgery, electrophysiology, and coronary intervention have been able to show a substantial reduction in costs through a series of competitive bidding strategies with vendors of various cardiovascular products.
30–33 Figure 8 shows the analyzed savings gained through negotiation strategies in various cardiovascular product lines over a period of 10 years.
 | Figure 8. Estimated Annualized Savings Gained through Combining Negotiation Strategies and Additional Product Lines. |
