A 40-year-old African American male patient, known to have homozygous sickle cell disease (SS genotype) and associated nephropathy, was admitted to our medical service in the summer of 2020 with a painful hemolytic crisis. He had presented with several weeks of progressive generalized weakness, generalized myalgias, and worsening dyspnea in the previous week. He had failed to take his prophylactic hydroxyurea for some time prior to presentation. Initial evaluation in the emergency department (ED) revealed lethargy and sedated level of consciousness with hypoxia and increased work of breathing. Following initial resuscitative measures in the ED, he improved. Pertinent admission laboratory data included sickle hemoglobin (HbS) 94.5%, hemoglobin A2 3.2%, mean corpuscular volume 103 fL, reticulocyte count 19.4% (baseline reticulocyte count of ~2.8%), white blood cell count 34.85×109/L with 85% neutrophils, platelet count 294×109/L, hemoglobin 4.6 g/dL, and hematocrit 13.1%. Peripheral smear revealed sickled red blood cells (RBCs). Chemistry revealed sodium 136 mmol/L, potassium 7.4 (3.5–5.0) mmol/L, glucose <20 mg/dL that quickly improved after 10% dextrose infusion, creatinine 7.20 mg/dL (baseline 1.5 mg/dL), bicarbonate <5 mmol/L, chloride 102 mmol/L, calcium 7.4 mg/dL, total bilirubin >40 mg/dL, phosphorus 11.6 mg/dL, conjugated bilirubin 38.7 mg/dL, unconjugated bilirubin 2.9 mg/dL, aspartate aminotransferase 374 IU/L, alanine aminotransferase 94 IU/L, alkaline phosphatase 418 IU/L, total protein 10.7 g/dL, albumin 3.6 g/dL, ferritin >6,000 ng/mL, creatine kinase 70 U/L, troponin I 0.042 (<0.034) ng/mL, ammonia 54 (<34) μmol/L, lactate dehydrogenase 3288 (313–618) U/L, N-terminal pro b-type natriuretic peptide 8940 (<125) pg/mL, partial thromboplastin time 31 s, prothrombin time 20.9 s, international normalized ratio 1.8, and lactic acid 11.6 mmol/L. The calculated MELD score was 40. Salicylate level was 1.7 mg/dL, and acetaminophen level was 14 μg/mL. Initial venous blood gas examination revealed pH 7.03, pCO2 38 mmHg, pO2 34 mmHg, TCO2 11 mmol/L, base deficit 19, and oxygen saturation was only 42%. Electrocardiogram (EKG) in the ED was abnormal and demonstrated sinus rhythm with prolonged QTc duration of 522 (<440) ms, together with inverted T waves in the lateral chest leads, V4–V6, consistent with true hyperkalemia (Figure 1). He had promptly received emergency therapies for hyperkalemia including intravenous (IV) calcium gluconate infusion, IV sodium bicarbonate infusion, IV 10% dextrose infusion with insulin, and IV furosemide. In addition, he was started empirically on IV antibiotics, vancomycin, and meropenem.
He was transfused with two units of packed RBCs and was promptly transferred to the Medical ICU. He quickly underwent emergency RBC exchange with therapeutic apheresis via a right femoral vein cannula, utilizing 1,999 mL of packed RBCs with a net fluid balance of 270 mL. Sickle hemoglobin (HbS) quickly dropped to 26.3% post-apheresis exchange. Initial nephrology consultation on admission had recommended correction of metabolic acidosis and treatment of hyperkalemia with more isotonic sodium bicarbonate infusions, insulin/glucose infusions, and the initiation of oral sodium zirconium cyclosilicate (SZC). He received one hemodialysis treatment on day 3 following evidence of encephalopathy which was subsequently blamed on drug toxicity from IV ketamine that was used for pain management.
Despite observing significant improvement of the acute kidney injury on chronic kidney disease in the first two weeks of this admission with much improved serum creatinine 2–3 weeks into the admission, as well as normal urine output, and stabilization of serum bicarbonate level to 22–27 mmol/L, the patient had exhibited persistent hyperkalemia (5.2–6.7 mmol/L) even with continued administration of SZC at 10 mg 2 times daily. The simultaneous trajectories of serum creatinine, platelet count, and serum potassium concentrations during the admission are shown in Figure 2. The patient had remained otherwise asymptomatic. Chlorthalidone, 25 mg daily, was added to manage the hyperkalemia without much success. Moreover, an EKG obtained in the 4th week of admission when the serum potassium that morning was 6.7 mmol/L was remarkably normal (Figure 3). At this point, as demonstrated in Figure 2, our patient had subsequently developed significantly progressive thrombocytosis, the result of previous treated sepsis. Admission leukocytosis of 34.85×109/L had decreased to 10.67×109/L in the 4th week of this admission. Nevertheless, usual therapies for hyperkalemia were again reinstituted in addition to the continued use of SZC and chlorthalidone.
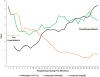 | Figure 2 Platelet Count, Blood Potassium, and Serum Creatinine |
From the foregoing observations and considerations, especially given the normal EKG shown in Figure 3 compared to the admission EKG in Figure 1 when he had true hyperkalemia with acute kidney injury and metabolic acidosis, for the very first time since this admission the possibility of pseudohyperkalemia was entertained. Consequently, later that same afternoon, following a conference call between the Nephrology and Internal Medicine Services, we repeated the simultaneous serum and plasma potassium measurements (after the emergency therapies for true hyperkalemia had been administered earlier that morning for a measured serum potassium level of 6.7 mmol/L). The measured simultaneous blood potassium levels were 5.8 mmol/L in serum versus 5.2 mmol/L in plasma. The reference range for blood potassium is 3.5–5.0 mmol/L. This confirmed the presence of pseudohyperkalemia secondary to the prevailing progressive thrombocytosis during this later part of the admission (Figure 2).6 Pseudohyperkalemia is diagnosed when the serum potassium concentration exceeds that of plasma by at least 0.4 mmol/L.6 Subsequently, the new potassium binder SZC was discontinued.
Five weeks after discharge, the patient was re-admitted to the same medical service this time with symptomatic painful sickle cell anemia crisis, fevers, cough with green sputum production, leukocytosis of 31.98×109/L, bilirubin 8.4 mg/dL, and chest radiograph that demonstrated bilateral multifocal patchy infiltrates consistent with pneumonia. Both HIV 1 and 2 and repeated COVID-19 RT-PCR tests were negative. He was started empirically on IV ceftriaxone, IV azithromycin, and IV vancomycin. Blood cultures grew methicillin-resistant Staphylococcus aureus within 15 hours in two out of two bottles, and IV antibiotics were de-escalated to 6 weeks of IV vancomycin administration. Admission serum creatinine was only slightly increased at 1.48 mg/dL, potassium was 5.7 mmol/L, but bicarbonate was 23 mmol/L. The patient responded well to IV antibiotics with resolution of the fever, and WBC had quickly dropped to 14.99×109/L after 2 days. Despite this quick overall clinical improvement, persistent hyperkalemia was again recorded throughout this second admission despite a low-potassium diet, IV furosemide, and the addition of oral fludrocortisone, 0.2 mg daily. Admission platelet count of 546 ×109/L had decreased to 314–450×109/L following IV fluids and IV antibiotics. This time round, simultaneous serum and plasma potassium levels were checked multiple times, and serum and plasma potassium concentrations were similar, indicative of true hyperkalemia. Hyperkalemia in the past had been related to pseudohyperkalemia associated with thrombocytosis. Factors contributory to true hyperkalemia were suspected to include sepsis accompanying the sickle cell crisis and intravascular hemolysis, concurrent exposure to heparin (subcutaneous enoxaparin 40 mg daily for deep vein thrombosis prophylaxis), and underlying sickle cell nephropathy with chronic kidney disease. The patient was restarted on SZC 10 g b.i.d. for 48 hours, and continued at 10–15 g daily. Serum potassium was maintained in the 5.3–6.3 mmol/L range throughout the hospital stay. The administration of SZC was to be continued post-discharge for 6 weeks with monitoring of serum potassium levels. To our knowledge, the patient has remained stable since discharge from the hospital.
