Donepezil, galantamine, and rivastigmine are drugs classified as reversible acetylcholinesterase inhibitors. The mechanism of action of these medications involves inhibition of the acetylcholinesterase enzyme leading to increased levels of the neurotransmitter acetylcholine, which in turn enhances cholinergic neurotransmission.1 Also, they can upregulate nicotinic receptors in the cortical neurons, promoting a neuroprotective environment. Therefore, it is believed that donepezil and other acetylcholinesterase inhibitors improve cognition due to increased acetylcholine concentrations in the hippocampus, raising hippocampal theta rhythm amplitude elicited by stimulation of the brainstem reticular formation.8
There are only a few case reports of myoclonus secondary to acetylcholinesterase inhibitors. We identified six cases after a review of the English-language literature, and we compared them with the present case (Table 1).2–7 A literature search was performed in Embase, Google Scholar, Lilacs, Medline, Scielo, and ScienceDirect, using a set of terms that included myoclonus, donepezil, rivastigmine, and galantamine.
 | Table 1 Case Reports of Myoclonus Secondary to Acetylcholinesterase Inhibitors. |
In 1987, Mayeux et al. reported the first case of myoclonus secondary to an acetylcholinesterase inhibitor.9 They described two patients with Alzheimer’s disease for whom physostigmine was prescribed. The first patient had increased myoclonus frequency with increasing physostigmine doses. Also, the authors described a dose adjustment in the second individual leading to a complete recovery of motor symptoms. These two reports are interesting because they provide different explanations for physostigmine-associated myoclonus. One reveals a significant dose-dependent response, and the other a threshold effect of an all-or-none mechanism. As a result, physostigmine is no longer prescribed due to neurotoxicity and high parasympathomimetic activity.
Ten years after the above reports with physostigmine, Abilleira et al. described a patient with middle-stage Alzheimer’s disease who presented with action myoclonus following tacrine use.10 They observed a recurrence of the twitching with tacrine rechallenge. In 2013, tacrine was withdrawn by the FDA due to safety concerns.
Currently, the most common acetylcholinesterase inhibitors prescribed for Alzheimer’s disease are donepezil, rivastigmine, and galantamine. Table 1 describes the case reports published related to myoclonus secondary to acetylcholinesterase inhibitors. There is no report of myoclonus secondary to rivastigmine. The mean age of the individuals that developed myoclonus was 76 years. Females were more frequently affected (57%). The majority of individuals had at least one comorbidity. The most frequent indication for acetylcholinesterase inhibitors was Alzheimer’s disease. Other indications were unspecified dementia and mild cognitive impairment. Myoclonus was multifocal in almost all cases, at presentation. Hernández-Fernández et al. described an interesting report of respiratory myoclonus, also known as diaphragmatic flutter, following galantamine therapy.3 Management consisted of discontinuation of the drug in all subjects. In some cases, benzodiazepines were prescribed, showing a shorter period of improvement of the motor symptoms compared to those who did not receive benzodiazepines. All the individuals recovered within 3 weeks.
Myoclonus secondary to acetylcholinesterase inhibitors is probably related to a primary cholinergic mechanism (Figure 1). In experimental studies, the reduction of acetylcholine function leads to improvement of picrotoxin-induced myoclonus.6 So, high levels of acetylcholine may be associated with involuntary twitching frequency. Also, donepezil increased extracellular dopamine release in the cortex and dorsal hippocampus in rat models. Surprisingly, norepinephrine levels in the prefrontal cortex were unchanged.1 Most cases occurred with donepezil and less frequently with other acetylcholinesterase inhibitors. This can be explained by the fact that galantamine and rivastigmine, compared to donepezil, have higher affinity and selectivity for acetylcholinesterase, preventing cholinergic adverse events at therapeutic doses.6,8
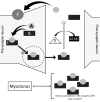 | Figure 1 Possible Pathophysiological Hypothesis for Explaining Myoclonus Secondary to Donepezil. |
